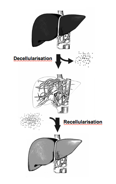
Our latest paper on "Monitoring of liver cell transplantation in a preclinical swine model using magnetic resonance imaging" has been accepted for publication in CELL Medicine (Part B of CELL TRANSPLANTATION). Authors are Nathanael Raschzok, Ulf Teichgräber, Nils Billecke, Anja Zielinski, Kirsten Steinz, Nora N. Kammer, Mehmet H. Morgul, Sarah Schmeisser, Michaela K. Adonopoulou, Lars Morawietz, Bernhard Hiebl, Ruth Schwartlander, Wolfgang Rüdinger, Bernd Hamm, Peter Neuhaus and Igor M. Sauer. The study was based on the excellent colaboration with the department of Radiology and the Institute of Pathology, both Charité - Campus Mitte, Universitätsmedizin Berlin, Berlin, Germany, the Centre for Biomaterial Development and Berlin-Brandenburg Centre for Regenerative Therapies (BCRT), Institute for Polymer Research, GKSS Research Centre Geesthacht GmbH, Teltow, Germany, the Department of Materials, ETH Zurich, Zurich, C Switzerland, and Cytonet GmbH, Weinheim, Germany.
Liver cell transplantation (LCT) is a promising treatment approach for certain liver diseases, but clinical implementation requires methods for non-invasive follow-up. Labeling with superparamagnetic iron oxide particles can enable the detection of cells with magnetic resonance imaging (MRI). We investigated the feasibility of monitoring transplanted liver cells by MRI in a preclinical swine model and used this approach to evaluate different routes for cell application. Liver cells were isolated from landrace piglets and labeled with micron-sized iron oxide particles (MPIO) in adhesion. Labeled cells (n = 10), native cells (n = 3) or pure particles (n = 4) were transplanted to minipigs via intraportal infusion into the liver, direct injection into the splenic parenchyma, or intra-arterial infusion to the spleen. Recipients were investigated by repeated 3.0 Tesla MRI and computed tomography angiography up to 8 weeks after transplantation. Labeling with MPIO, which are known to have a strong effect on the magnetic field, enabled non-invasive detection of cell aggregates by MRI. Following intraportal application, which is commonly applied for clinical LCT, MRI was able to visualize the microembolization of transplanted cells in the liver that were not detected by conventional imaging modalities. Cells directly injected into the spleen were retained, whereas cell infusions intraarterially into the spleen led to translocation and engraftment of transplanted cells in the liver, with significantly fewer microembolisms compared to intraportal application. These findings demonstrate that MRI can be a valuable tool for non-invasive elucidation of cellular processes of LCT and - if clinically applicable MPIO are available - for monitoring of LCT under clinical conditions. Moreover, the results clarify mechanisms relevant for clinical practice of LCT, suggesting that the intra-arterial route to the spleen deserves further evaluation.